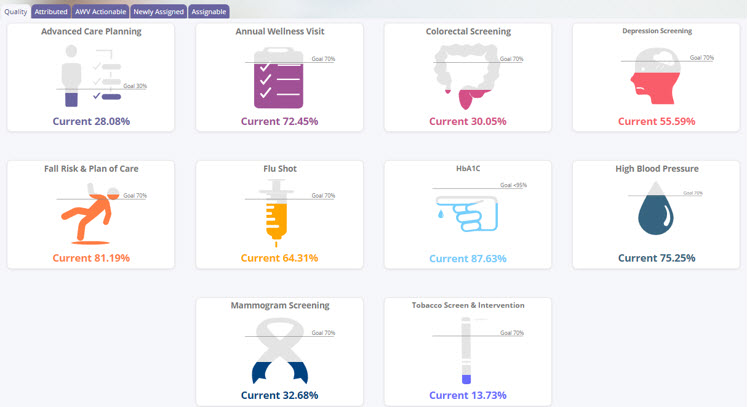
Monitoring the health of your population and doing preventative care is essential in keeping your population healthy and reducing unnecessary costs. Our solution offers 13 prebuilt measures focusing on high impact measures; with the ability to expand them based on contract specific terms. For ACO’s the completion of quality metrics is an established CMS requirement and can affect your shared savings distributions.
Our quality data includes last measure dates, performance indicators and met performance vs. not required (using NQF denominator/numerator logic). Track your performance on an easy-to-understand dashboard.